How Does Diabetes (Type-2) Affect the Digestive System?
At early stages of type-2 diabetes, the disease may not cause symptoms. But if left uncontrolled, it may get worse and cause complications affecting other organs of the body, including the digestive system.
Diabetes affects the mechanism of the body in using glucose (sugar). We need glucose for energy. But with diabetes, glucose in the bloodstream cannot be effectively converted into energy. As a result, the blood sugar level increases. In time, the disease may cause a cascade of other health problems!
It’s very crucial for diabetics to manage and control their blood sugar level. More episodes of high blood sugar, more likely for diabetes complications to occur.
In other words, regular blood sugar tests are required. This can help monitor the level and take appropriate steps immediately if the level is abnormal!
There are several choices to help check and monitor blood sugar level:
Gastroparesis may be the most common digestive problem that affects patients with diabetes. Athough it is relatively more common in type-1 diabetes, sometimes it also affect people with type-2.
The condition would make your stomach work slower than usual in emptying stomach contents – this condition is also called as a ‘delayed gastric emptying’. As a result, the stomach is no longer to empty itself in a normal way.
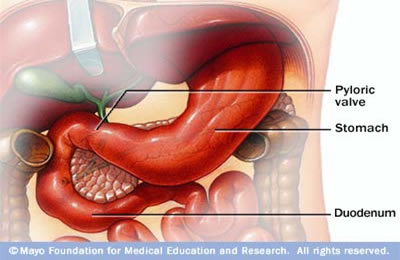
Below is the picture (credit to Mayo Clinic) that describes the condition:
The stomach (gastric) is a strong muscular sac. The size is about similar to a small melon, but it can expand to respond on what you drink and eat.
Once it pulverizes the food, the contractions of strong muscular (these contractions familiar known as ‘peristaltic waves’) will encourage the food move forward to the pyloric valve, which then eventually go to the duodenum (the upper section of the small intestine).
Poor-controlled blood sugar in people with diabetes will increase the risk of the vagus nerve damage. It may also damage the blood vessels that supply essential nutrients and O2 (oxygen) to the nerves.
The vagus nerve is very crucial for your digestive system. It is responsible to regulate the way of digestive system to work and make the muscles work.
If the vagus nerve is no longer to work properly – this can significantly affect the rhythm of stomach in emptying itself naturally. As a result, foods that you eat is not properly processed in the stomach and also not distributed to the gut.
Although gastroparesis can be treated (e.g. with appropriate diet, medicines, insulin management, or even with a feeding tube in severe case of gastroparesis)), delayed digestion would also cause a problem in the management of diabetes. Diabetics with this digestive problem are likely to become very poor in controlling their blood sugar.
It’s not always associated with poorly controlled diabetes. Sometimes, it may also be a consequence of the following conditions:
- Scleroderma and Amyloidosis – fortunately, both are rare health conditions.
- Parkinson’s disease.
- After stomach surgery, particularly certain surgery that can be potential to injury or affect the vagus nerve.
- Multiple sclerosis.
- Abusing drugs (such as abusing narcotics)
- Medications, such as certain antidepressants.
The symptoms of this digestive problem in diabetes may include [reference]:
- Weight loss and lack of appetite.
- Easier to feel full during and after eating.
- Nausea that may be followed by vomiting (vomiting for undigested foods).
- Abdominal bloating.
- More difficult to control your blood sugar.
- Gastroesophageal reflux (heartburn).
It’s important to treat gastroparesis in diabetes. If left untreated, it may cause some of the following complications: